Taylor CapizolaGHTC
Taylor Capizola is a program assistant at GHTC who supports GHTC's communications and member engagement activities.
In this regular feature on Breakthroughs, we highlight some of the most interesting reads in global health research from the past week.
Sanofi, a major vaccine developer, ceased their Zika vaccine program, highlighting how difficult it is to develop an effective vaccine for Zika. The US Biomedical Advanced Research and Development Authority reduced funding to Sanofi for the vaccine program last month, and Sanofi announced in early September it will no longer seek funding to continue its vaccine research. Smaller companies are in clinical stages of testing different Zika vaccine candidates, but Sanofi was the first major US pharmaceutical company to begin research on a potential vaccine for the virus.
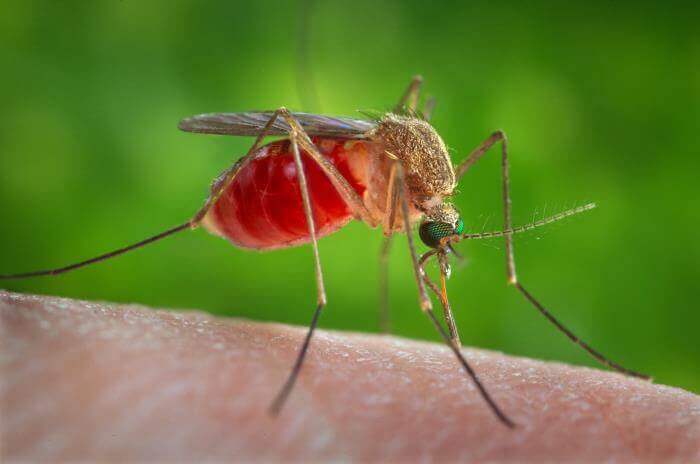 A female Culex quinquefasciatus mosquito (CDC/ James Gathany)The Infectious Diseases Data Observatory, a research observatory based out of the University of Oxford in the United Kingdom, is developing a data-sharing platform to compile and share Ebola data to aid in the response to future outbreaks. Researchers are seeking to engage
local African leaders in the platform's creation to provide cultural context and ensure the resulting system improves the capacity of African researchers
to conduct research in outbreak scenarios. Organizers agree that developing the platform now—during a period of no active outbreaks—is
critically important, as having the platform available for aid workers and medical professionals before the next Ebola outbreak may aid in saving lives.
A female Culex quinquefasciatus mosquito (CDC/ James Gathany)The Infectious Diseases Data Observatory, a research observatory based out of the University of Oxford in the United Kingdom, is developing a data-sharing platform to compile and share Ebola data to aid in the response to future outbreaks. Researchers are seeking to engage
local African leaders in the platform's creation to provide cultural context and ensure the resulting system improves the capacity of African researchers
to conduct research in outbreak scenarios. Organizers agree that developing the platform now—during a period of no active outbreaks—is
critically important, as having the platform available for aid workers and medical professionals before the next Ebola outbreak may aid in saving lives.
A new, low-cost tool has been introduced in disadvantaged areas to treat newborn asphyxia. Newborn asphyxia is highly prevalent in low-resource settings, with about 20 percent of all newborn deaths in India caused by the condition. Therapeutic hypothermia—which reduces an infants body temperature—is a common treatment, but hypothermia-inducing machines are typically too costly for low-resource settings. Dr. Niranjan Thomas of Vellore, India created the MiraCradle, a fast-acting, low-cost device made of several phase changing materials—substances that absorb and release thermal energy—that is used as a regulation agent to keep a newborn hypothermic. The MiraCradle is currently being used in about 125 hospitals throughout India and South Africa.