Kat KelleyGHTC
Kat Kelly is a senior program assistant at GHTC who supports GHTC's communications and member engagement activities.
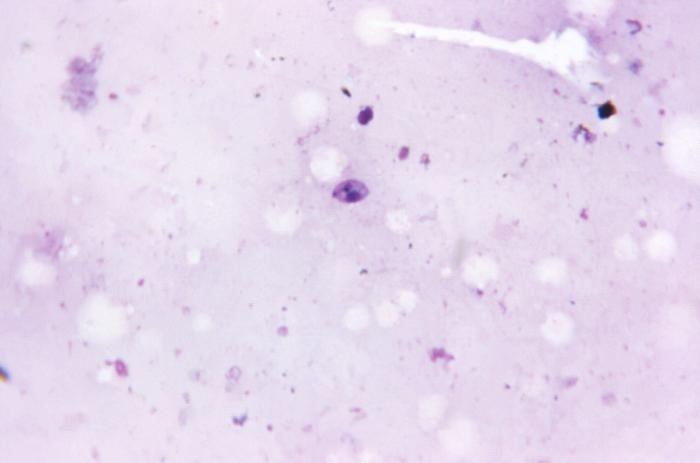
The Drugs for Neglected Diseases initiative (DNDi)—a member of the GHTC—is partnering with pharmaceutical companies Eisai Co., Shionogi & Co., Takeda Pharmaceutical, and AstraZeneca to accelerate early-stage research for drugs against Chagas and leishmaniasis. The project, known as the Drug Discovery Booster, will enable DNDi to search through all the pharmaceutical companies’ vast libraries of chemical compounds simultaneously. DNDi will provide each company with a ‘seed’ compound which has shown some ability to combat the parasites responsible for the diseases, and the companies will subsequently scan their libraries for similar, and potentially more promising, compounds. DNDi will then test the compounds identified by the pharmaceutical companies and pick a new seed compound from the results. This process will be repeated up to three times. The GHIT Fund—a member of the GHTC that subsidizes research and development for neglected tropical diseases—is supporting the involvement of the three Japanese pharmaceutical companies.
The World Health Organization updated its medical eligibility criteria for contraceptive use last week, adding long-acting, hormonal contraceptives to the list of recommended contraceptives. The list is widely used by medical practitioners to identify the best contraceptive methods for their patients and by policy-makers in shaping national strategies that determine the availability of different methods within their countries. Under previous guidelines, health professionals were advised not to prescribe hormonal contraceptives to women within the first six weeks after giving birth. Revising that recommendation is expected to increase contraceptive access for new mothers, enabling healthy birth spacing and ultimately reducing maternal and child mortality. This is particularly important in light of the results of a recent study in Contraception across 21 low- and middle-income countries, which indicates that more than half of pregnancies in women who have previously given birth occur too soon after delivery to be safe.
An experimental diagnostic known as VirScan can identify virtually every virus a person has ever been exposed to using just a drop of blood. VirScan detects antibodies—proteins that the immune system makes to combat infection—and has been tested on 569 people across the United States, South Africa, Thailand, and Peru. The test costs US$25 and currently takes two days to two months to complete. However, the researchers believe that if a company were to lead and streamline its use, the process could reliably be cut to two to three days. Initial results indicate that the average person has been exposed to 10 virus species, however, those in the United States have generally been exposed to fewer viruses, which could be attributable to “differences in population density, cultural practices, sanitation or genetic susceptibility.” VirScan could be used to identify viral causes or catalysts of chronic or autoimmune diseases, as well as global disease patterns.